聯絡我們:+852 2367 6116
24小時中風熱線:+852 8107 1616
Acerca de
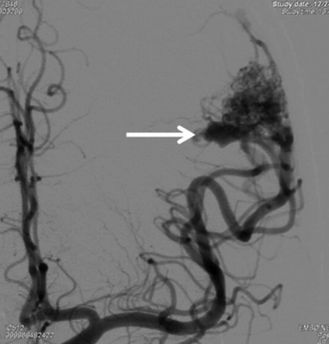
腦動靜脈畸形血管瘤
簡介
普羅大眾都以為中風和年齡有著必然的關係,然而這是不正確的。任何年齡,即使是小孩也有機會中風,皆因中風是腦血管疾病所致,而我們每個人,無論任何年紀也有機會患上先天性或後天性的腦血管病變。這則簡介與治療概覽提供了一些關於腦動靜脈畸形血管瘤的基本知識,同時就病人及其家屬關心的一系列常見問題給予解答。
腦動靜脈畸形血管瘤(Cerebral Arteriovenous Malformation - AVM)是先天性的腦血管病變,患者的年齡廣泛,由四歲小童以至八十多歲的老人家也有。先天性的腦動靜脈畸形血管瘤一旦破裂,能導致嚴重的出血性中風,對病人的腦神經功能及身心之殘害影響至鉅,亦會令家庭親人背負着沉重的身心及經濟負擔。

動靜脈畸形血管瘤
(Cerebral Arteriovenous Malformation - AVM)
什麼是腦動靜脈畸形血管瘤?
腦動靜脈畸形血管瘤是一種先天性的疾病,致病原因不明,亦沒有遺傳基因導致。患者胎兒時在母親體內之腦部發育時,動靜脈畸形的問題已經形成。在腦部某處血管不正常的畸形血管組織。畸形血管組織欠缺了正常的微絲血管系統,讓腦動脈血管與靜脈血管直接相連。
正常人體腦部的供血,是由心臟及頸項的大血管,再經由腦部的四條主動脈血管,經過分支血管再流至多條極之細小的微絲血管系統。血液裏的氧氣和養份會經過微絲血管壁之滲透去供養腦細胞,之後血液就會經過靜脈血管系統排走,回流到頸項之靜脈,繼而流回心臟,作為一個循環。
除了提供氧氣和養份給腦細胞之外,微絲血管的另一功能就是作為流入動脈血管內的血液壓力之緩衝。可是,先天性動靜脈畸形血管瘤的中心處,天生就是缺少了正常應該有的微絲血管系統,令到靜脈在沒有緩衝下承受著來自動脈血液的巨大壓力,令靜脈血管變得曲張脹大,其血管壁亦變得脆弱,容易破裂出血,繼而引發出血性中風。
腦動靜脈畸形血管瘤患者之性別、年齡分佈和症狀
-
沒有任何症狀:
大多數患者由出生至到畸形血管瘤爆破之前,都沒有任何症狀。
-
腦部供血不穩之症狀:
畸形血管可以令到其附近之腦細胞的接受供氧比例降低,因而引發一些神經症狀,例如:偶爾說話困難不清、肢體麻痹無力、視力不穩、甚至乎是癲癇症發作。
-
出血性中風:
先天性腦動靜脈畸形血管瘤之患者以女性較多,其涵蓋的年齡層廣泛,由四歲小童以至八十多歲的老人家也有。雖然腦動靜脈畸形血管瘤每年爆破的風險少於1%,但它卻是兒童、年輕人、孕婦、身體健康人士出血性中風的主因之一,病發的大多數處於 10多歲至40多歲的年齡層。懷有先天性腦動靜脈畸形血管瘤的人通常由小到大都沒有任何症狀,直至血管瘤爆破時才有劇烈頭痛、頭暈、噁心、嘔吐、神經功能失調、意識混亂、癲癇症發作、甚至昏迷的緊急症狀。
腦動靜脈畸形血管瘤的每年爆破機會比率
雖然血管瘤每一年爆破的機會率少於1%,然而若果病人的年紀越小,其一生所逐年累積的爆破風險亦相繼較大。
腦動靜脈畸形血管瘤如何被診斷?
由於懷有先天性腦動靜脈畸形血管瘤的人通常由小到大都沒有任何症狀,直至血管瘤爆破時才有緊急症狀,因此任何人在沒有任何症狀下,預先做腦部及其血管結構的詳細身體檢查,事先診斷自身有否患有先天性或後天性的腦血管病變,好讓隱藏腦內之計時炸彈爆破及引致嚴重出血性中風之前,計劃應對及選擇治療方案,做好預防性的治療,便可以大大減少許多悲劇和遺憾了。
篩查腦動靜脈畸形血管瘤的詳盡身體結構檢查
-
磁力共振(MRI)和磁力共振血管造影(MRA)
磁力共振是一種「無輻射、無創傷、無痛楚」的掃描造影技術,與帶有輻射的X光或電腦斷層掃瞄(CT scan)大有不同。先進的磁力共振機不單止無需注射顯影劑,亦能做到 3D三維立體腦血管造影的效果,又能夠準確、清楚地照出腦動靜脈畸形血管瘤的位置及其與正常腦組織的關係。
此外,磁力共振亦可掃描人體全身不同部位,亦可為沒有病徵人士進行全身體內結構的詳盡篩查,偵測潛在身體結構內裡中風或癌症之風險。
-
電腦斷層掃描血管造影(CTA)
電腦斷層掃描血管造影(CTA)牽涉輻射和靜脈注射顯影劑,雖然不是一般身體健康篩查的首選造影檢查,但它能提供更多資訊,讓神經血管外科醫生在選擇醫療方案時作參考。
-
動態 及 3D 三維立體數碼遞減腦血管造影( Dynamic 3D Digital Subtraction Cerebral Angiogram DSA)
雖然是微創入侵性的檢查,亦牽涉輻射和注射顯影劑,但它是神經血管外科醫生選擇治療方前必須的,而且是黃金規格之最終檢查,能夠讓醫生全面掌握腦部血管:由動脈到微絲血管,以至靜脈血管內血液之動態流向和速度,有著全面的資訊。此外DSA能夠讓醫生知道畸形血管有沒有在短時間內爆破之風險,從而為病人作出一個最佳醫療方案和時間期限。

腦動靜脈畸形血管瘤的治療方案
目前的治療方案:
-
保守觀察:
若患者完全沒有症狀,又或者有症狀但是年紀老邁、身體健康嚴重不佳、或個別情況下醫生認為進行任何治療會比不治療的風險較高,醫生一般都會以保守性治療觀察。
-
微創顯微鏡腦血管外科切除手術 (Minimally Invasive Microscopic Excision):
手術是在3D三維立體電腦導航的指導下進行,如有需要,神經血管外科醫生亦 會使用運動神經腦皮層反射和連續腦功能監測系統,在顯微鏡下,除了以徹底切除動靜脈畸形血管瘤和去除血腫為目的之外,醫生亦會用盡一切方法完好地保護病人腦部的神經功能,以免受損。手術的成功率取決於腦動靜脈畸形血管瘤的大小、位置、複雜程度,以及負責手術的醫生之相關經驗。
-
血管栓栓塞手術(Endovascular Embolisation):
視乎臨床情況,導管堵塞手術療法可以獨立進行治療,或可以應用在顯微鏡手術切除前、或放射治療前進行,用以減少腦動靜脈畸形的體積和範圍。
神經血管外科醫生會在病人大腿腹股溝上的動脈,以針孔傷口,利用極微細的導管,經過病人體內的大動脈,在X光導航下將導管遊走至病人大腦的血管,醫生然後會在動靜脈畸形的血管中,注入極微細的鈦金屬絲、塑膠珠球或是特製膠水,用以栓塞供養畸形血管的動脈和畸形血管的中心。腦血管導管堵塞手術之風險,主要在於手術進行時意外地傷及正常和畸形血管,令其堵塞或破裂出血,引致缺血性或出血性中風。手術之另一風險就是在過程中意外地將畸形血管排出血液的靜脈血管過早被堵塞,令到畸形血管內的血液被排出,血液壓力急速上升而令血管瘤爆破。
-
放射線療法(Radiosurgery ):
放射治療不需要麻醉,治療是從多個角投放輻射線,高能量的輻射線會集中在畸形血管上,令到不正常的畸形血管隨著歲月,慢慢地在兩至三年的長時間內連續漸進閉塞,令到血液無法通過畸形血管而是流會回正常的血管中,畸形血管瘤消失後,病人出血性中風的風險就可以大幅降低了。
放射治療適用於:
- 畸形血管瘤大小少過3厘米
- 血管瘤在腦部的位置太深入
- 血管瘤在腦部的位置太過接近重要神經功能部位
- 血管外科醫生經過評核後認為若果以血管堵塞術或顯微鏡切除手術,所牽涉的風險較大
放射治療之風險:
- 雖然不用麻醉和做手術,但由於放射治療涉及輻射,而輻射線必須穿過正常腦組織才能到達畸形血管瘤,難免會對附近的腦細胞和血管組織,造成短期或長期的影響。
- 如果放射治療的位置不夠精準,可以造成畸形血管之靜脈部份過早閉塞,令到血液只會經由動脈血管流入畸形血管,而不能經過閉塞了之靜脈血管流出,令到畸形血管瘤內血壓提升而爆破,引致出血性中風。
放射治療的系統選擇:
- X光刀 (X-Knife)
- 伽瑪刀 (Gamma Knife)
- 數碼導航刀 (Cyberknife)
影響治療決策的因素
依據美國中風協會的治療標準(ASA Guideline),我們可以依美國神經血管外科醫生 Professor. Spetzler-Martin的研究將AVM的危險程度分成五級(見下圖),來區分治療的方法:
-
低度危險(第1、2級)的AVM
神經血管外科醫生一般會使用微創顯微鏡腦血管外科切除手術 (Minimally Invasive Microscopic Excision)來治療,若是畸形血管瘤的位置 涉及重要腦神經功能之部位,醫生可以考慮使用放射療法(Radiosurgery)。
-
中度危險(第3級)的AVM
可以在微創顯微鏡腦血管外科切除手術後,再施以血管栓塞術 (endovascular embolisation)來作治療。
-
高度危險(第4、5級)的AVM
若任何治療方案都會太危險,一般醫生會以保守性療來持續觀察

三種放射線療法的差異如下以供參考:

腦動靜脈畸形血管瘤的併發症
-
出血性中風:腦動靜脈畸形約佔所有出血性中風2%,是常見兒童或年輕人中風的主因之一。腦動靜脈畸形會容易引起血管破裂,引發顱內出血,對於特定類型的腦動靜脈畸形,或曾有顱內出血過,出血性中風的風險還會再增高。
-
腦部缺氧:因為腦動靜脈畸形會讓氧氣進入腦部的比例降低,此時會引發一些其他的症狀,例如:說話困難、虛弱、四肢麻木、視力不穩定或喪失。
-
腦部損傷:有些腦動靜脈畸形會讓部分血管管徑變粗,壓縮到部分的大腦,可能會引起腦部的局部損傷。有時也會造成液體積聚在腦部的特定區域,引起腦積水狀況。
相關案例
案例(一):孕期中的女性畸形血管瘤突然爆破
兩個分別15及16歲的少女,一向健康、沒有頭痛症狀,兩個案例分別在懷孕初期及中期,隱藏腦內之計時炸彈: 先天性的腦動靜脈畸形血管瘤突然爆破及引致嚴重出血性,劇烈頭痛後急速昏迷休克。在緊急腦外科開顱手術清除瘀血及減低顱內壓後,神經血管外科醫生等待3個月讓腦腫脹消退後,再以微創顯微鏡血管瘤切除手術根治,兩名少女和他們的小孩完全康復,沒有任何後遺症。
另一案例是一位39歲的懷孕後期的女士,就發生在嬰兒要出世而作動的一晚,她的丈夫英勇果斷的把她和嬰兒從鬼門關中拯救出來,嬰兒現在已是一個健康和可愛的孩子了。 無奈39歲的女士,由於動靜脈畸形血管瘤破裂引至嚴重的大腦功能損傷卻變成了植物人,醫生嘗試用過每一種治療方案亦不果,在醫院臥床了五年才去世。
.jpeg)




案例(二):四歲稚子大腦神經永久損害
四歲小朋友,出生以來一切健康正常,沒有任何症狀,有一天隨母親逛街時突然感到頭部劇痛,然後急速昏迷。送到醫院證實是先天性大腦動靜脈畸形血管瘤爆破引致嚴重出血性中風。他雖然從鬼門關被拯救出來,但即使經過五年多的醫治也不能逆轉中風對大腦神經的永久損害。如今小孩仍然患有嚴重殘疾,需要長期臥床,也無法與人溝通。
案例(三):血管瘤破裂流血導致肢體無力
49歲的女士,接種疫苗後2週感到左腿無力,雖然看了中醫和骨科醫生,更做了脊柱磁力共振MRI造影,仍然找不到原因。腦血管外科醫生經過臨床評估後為她進行了3D三維立體磁力共振腦血管造影,顯示其大腦都有先天性動靜脈畸形血管瘤並且已經少量出血,瘀血壓著她右腦負責控制左腿功能的位置。在3D三維立體電腦導航、運動神經腦皮層反射和連續腦功能監測系統下,神經血管外科醫生在顯微鏡下徹底切除血管瘤和去除瘀血,病人腦部的神經功能得以完好恢復。手術後,病人左腿的力量恢復正常。

手術在三維立體電腦導航指導下進行。


使用運動皮層映射和連續腦功能監測系統進行手術。
案例(四):畸形血管瘤出血引起嚴重腦癲癇症發作
一名37歲女士被發現在家中暈倒、喪失意識,被送入公立醫院。病人和家屬獲告知CT電腦掃描、腦電波圖和所有血液化驗結果一切正常,醫生仍然沒有臨床線索來確定她暈厥的原因。於是病人出院後諮詢腦血管外科醫生意見,醫生審查公立醫院的血液檢查報告時發現病人血清肌酶素曾經非常高,表示她暈倒、意識不清的原因是嚴重強直陣攣性腦癲癇症發作。醫生於是為她進行3D三維立體磁力共振腦血管造影,造影顯示病人左前額大腦腦葉藏有一個3 cm的先天性動靜脈畸形血管瘤,並有少量最近出血的現象,是她失去意識和腦癇症的原因。動態 3D 三維立體數碼遞減腦血管造影(Dynamic 3D Digital Subtraction Cerebral Angiogram DSA)確定血管瘤內血液的流動模式。在4小時的顯微鏡下,血管外科醫生在血管瘤旁邊的腦部看到血鐵黃素的舊有殘留血液,血管瘤和瘀血均被徹底移除。病人腦部神經功能得以完好保全,手術後兩天出院,10年來癲癇症再沒有發作。
案例(五):放射治療導致血管瘤靜脈部份過早閉塞,令血管瘤爆破
當年42歲的家庭主婦,與家人到深圳作全身檢查時,發現腦裏有一個先天性的腦動靜脈畸形血管瘤。回港後,該女士到公立醫院求醫,醫生告知她應採取觀察和保守治療方案。可是,在家人的勸告下,病人遠赴廣州進行了X光刀放射治療。手術後回港不久,病人在 凌晨時份 睡夢中口吐白沫,不醒人事,被送往附近的公立醫院。在緊急腦外科開顱手術清除瘀血及減低顱內壓後,神經血管外科醫生再作詳細調查,懷疑是放射治療的位置不夠精準,造成畸形血管之靜脈部份過早閉塞,令到血液只會經由動脈血管流入畸形血管,而不能經過閉塞了之靜脈血管流出,令到畸形血管瘤內血壓提升而爆破,引致出血性中風。雖然病人幸運地被救回性命,但受損的腦神經區域卻令她喪失說話能力(俗稱「失語症」)及喪失右手的活動能力。


案例(六):趁危機引爆前拆除它
兩位分別是16歲的少年和56歲的男士,在沒有任何徵狀時做了詳盡的腦及腦血管結構檢查,3D三維立體磁力共振腦血管造影顯示兩人的大腦都有先天性的腦血管動靜脈畸形血管瘤,在血管外科醫生建議下,經過一段時間的觀察和保守治療,其後利用了微創腦血管導管堵塞手術、加上放射治療,畸形血管瘤得到了有效根治,病人與生俱來的大腦計時炸彈得以拆除,消除了他們將來出血性中風的風險。


3D 三維立體腦血管造影顯示,左邊大腦有先天性的腦血管動靜脈畸形 (AVM)。